Constipation affects up to 1 in 7 of us and can be a source of great distress. In this article, we’re going to explore what your constipation is all about and four ways to improve your flow.
Definitions:
• Colon: the large bowel
• Sphincter: a ring-shaped muscle that relaxes or tightens to open or close a passage in the body
• IBS-C: irritable bowel syndrome of constipation subtype
• Muladhara chakra: mula meaning 'root' and 'adhara' meaning base. In yoga, it is said that this energy centre is associated with safety, security and our ability to let go of fear
What is the colon?
Before diving in, I think we should take a moment to remind ourselves what this incredible organ does for us each and every day.
The colon is a 1.5 metre long section of our digestive system responsible for absorbing water and salt, whilst storing and eliminating our waste. In order to perform this function the colon relies on a complex network of nerves and muscles as well as trillions of microbes.
And like most organs in our body - it’s not until something isn’t working that we really notice and appreciate all that it does for us.
Are you really constipated?
It’s important to establish what a normal and healthy bowel habit is for you.
Bowel habits vary significantly from person to person. Some people go once every couple of days, and others go three times per day. There is no true normal pattern. However, most people tend to feel it is abnormal when their bowel movements are less than 3 times per week or they cause pain, discomfort and negatively impact their quality of life.
Signs of chronic constipation include two or more of the following over the last three months; hard or lumpy stools; straining; a feeling of not being completely empty; or less than three bowel movements per week.
Note: If you are bleeding from your back passage, please see your doctor. While piles or haemorrhoids are extremely common in constipation, it should always be checked out.
Remember - nearly everyone experiences changes in their bowel habit due to certain foods, when we travel abroad and for women during menstruation.
The three mechanisms of constipation
I would like you to think of your colon as both a river and a reservoir.
Here are the three mechanisms by which your colon can run into problems - leading to chronic constipation:
1. The wave machine
Our colon makes wave-like movements to move the stool along. These waves are linked to our circadian (roughly 24-hour) rhythms, which is why so many of us open our bowels first thing in the morning or after meals and why many people get constipated when they travel around the globe!
Constipation can be caused by a reduction in the number or strength of these wave-like movements which are responsible for motion along the river bed. Perhaps your colon has always been a little slow to move or has become sluggish over time and this leads to what we call slow transit.
2. The sphincter muscles
Our rectum (back passage) is the so-called reservoir and holds onto our stool via the incredibly well-timed co-ordination of our anal sphincter muscles - think of them like a dam preventing overflow! Constipation can be caused by a lack of coordination in these muscles which can affect their ability to relax and release stool. Causes of this can include damage to the sphincters during childbirth or surgery.
3. The pelvic floor muscles
Finally, constipation can occur when our pelvic floor muscles are not intact, strong and flexible. This can be caused by weakening during pregnancy, trauma or simply not having worked at them throughout our lives to make them strong and responsive.
Four ways to improve your constipation
1. The 2 F’s - Fibre & Fluid
I think everybody knows about the importance of fibre these days. A lot of people, however, think about the insoluble forms like bran flakes and green leafy vegetables, which can actually irritate the gut lining. There is a another very important fibre called soluble fibre which forms a soothing gel over the colon lining and together with insoluble fibre bulks up the stool. If you eat plenty of fruits and vegetables you will be getting a good combination of both fibres.
Yet some soluble fibres are also fermentable, which may worsen bloating and abdominal distension in people who have IBS-C. If this is you, I would recommend going for foods that have the highest percentage of soluble fibre yet are non-fermentable, for example: oats, linseeds/flaxseeds and the flesh of low fodmap fruits and vegetables.
To help fibre do its job, we also need plenty of fluids. If you increase your consumption of fibre then increasing your consumption of water (i.e. to 2 litres per day) is essential.
Top Tip - the best sources of combined soluble and insoluble fibre:
(a) Flaxseed (milled or crushed): an ancient plant crop from Southern Europe and Asia which contains an oil rich in omega-3 fatty acid, alpha-linolenic acid. Sprinkle on your breakfast cereal or over yoghurt – approx. 1 x tablespoon per day will do.
(b) Kiwi fruit: a berry of two varieties – green or gold. Kiwis are high in vitamins C, E, K and micronutrients potassium, folate and phytochemicals but especially fibre! This study trialled a dose of two kiwi fruit per day (contains about 9g of dietary fibre) and found significant impacts on stool frequency and consistency, confirming it “can be used as a dietary alternative to laxatives in mild constipation”

But what if dietary changes don’t do the trick?
2. Short-term laxatives
If dietary changes don’t do the trick, the short-term step would be to try laxatives.
Now, many of my patients avoid taking regular laxatives because they feel they will become dependent on them. This is simply not the case – I am here to tell you that laxatives do not make your bowel lazy! It is far more preferable to keep your internal river moving smoothly by taking regular laxatives than to let yourself teeter on the edge of discomfort, as this can cause other issues.
Generally speaking, there are two types of laxatives: stimulants (e.g. senna / senokot) and stool softeners
(e.g. sodium docusate / dulcolax). Stimulants generate stronger wave-like movements of the colon whereas stool softeners actually soften your stools to make them easier to pass. Then there are suppositories and enemas which are most effective if you have symptoms such as straining or incomplete emptying.
Top tip – start with the choice of laxative which best treats what you feel is the issue for you (i.e. slow transit e.g. stimulants; or hard stools e.g. stool softeners; or incomplete emptying e.g. suppositories) and then add a second type because they work better together.
3. Behavioural therapy – with a Yogic spin!
Before the advent of modern toilets, our ancestors used to squat on the ground to empty their bowels. Little did we know that we have gone backwards instead of forwards!
The muscles of our pelvis have a significant role to play in our ability to poo normally, specifically - our puborectalis muscle which forms something called the anorectal angle.
Sitting on a modern toilet the anorectal angle is closed and so your poo has to navigate a tight corner to make its exit! When we assume a squatting position (i.e. raise our knees above our hips) we open the anorectal angle by relaxation of the puborectalis muscle and the pelvic floor – thus enabling a straight and easy passage of poo.
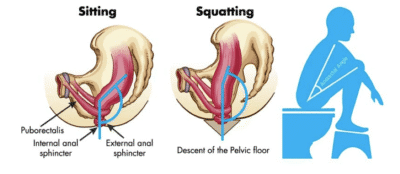
https://toiletfound.com/toilet-squatting-rear-story/
Top tips:
(a) use a foot stool or ‘squatty potty’ to open up the anorectal angle
(b) place your elbows on your knees and relax your shoulders
(c) breath evenly, do not your hold your breath (see my breathing videos here)
(d) when you push down, exhale and sustain the push towards your thighs for 10 seconds then relax for 10 seconds – avoid straining
(e) sit for a minimum of 7 minutes and a maximum of 10 minutes – then wipe and walk away!
Now for the Yoga posture to encourage relaxation of the pelvic floor muscles :
Happy Baby pose (Ananda Balasana)

Here are the five steps to practicing:
(1) lie on your back and hug your knees into your chest, take a few deep breaths to settle down.
(2) take hold of the outside edges of your feet with your hands (you can have your arms on the inside or outside of your legs)
(3) open your knees slightly wider than your torso and flex the soles of your feet to the sky, position each ankle directly over your knee
(4) gently push your feet into your hands to create some resistance and take gentle breaths for 5 minutes or so
(5) release your arms and hug your knees back into your chest for a few breaths.
The word constipation comes from the Latin constipatio which means ‘contraction of body tissues.’ The question is, when you suffer from constipation, does contraction only occur in the bowel? What about the pelvic floor muscles? What about … the mind?
4. Identifying the ‘root’ of the problem
Let’s face it, there is nothing more satisfying than having a good bowel movement! This is because emptying our bowels involves relaxation of the pelvic floor muscles via the vagal & pudendal nerves which communicate a relaxation response to the whole body.
The ancient Yogic texts describe several anatomical points located along the central axis of the body – so-called chakras, believed to provide a passage for energy to enter and exit the body. Interestingly, they do in fact loosely correspond to western anatomical points.
In this study, Muladhara chakra was found to be in close association with the inferior hypogastric plexus – a collection of nerves supplying our pelvic organs. In yoga, it is said that our root chakra is associated with our sense of safety, security and our ability to let go of fear.
So if our basic emotional needs are not met, eastern philosophy would suggest that we may develop issues in our pelvic organs - including the bowel. Or perhaps it is the other way around - if we suffer from constipation, can we feel unsafe, insecure or fearful?
Top tip: Managing a physical issue holistically involves addressing the underlying cause. Be open and explore the role your mental health plays in constipation, which may begin close to these ancient roots.
Tying it all together
The above tips and tricks are meant to be tried in combination as they target different areas of the pelvic floor and colon that could be an issue. Yet it may come down to the places you contract where you could do with relaxing.
If you feel you have tried everything and are close to giving up, my advice is to engage with mind-body tools which encourage your gut and nervous system to go with the flow - like Yoga for IBS: my monthly programme or Gut-directed hypnotherapy - so get in touch with me to discuss more.
In the meantime, I wish you all - happy elimination!

